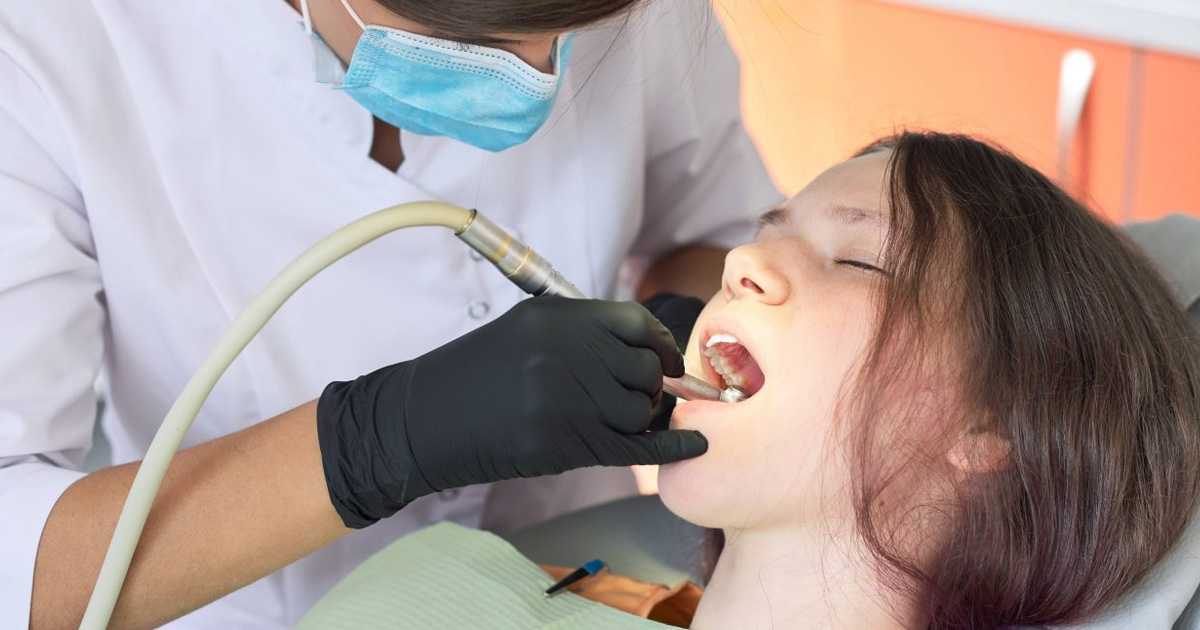
We provide a wide range of oral surgery and periodontal surgery services. Wisdom teeth removal, simple extractions, surgical extractions, gum grafting, and bone grafting are all common procedures at our office. Mint Hill, Matthews, Indian Trail and surrounding Charlotte-area families have trusted our doctors for their oral surgery needs for over 40 years.
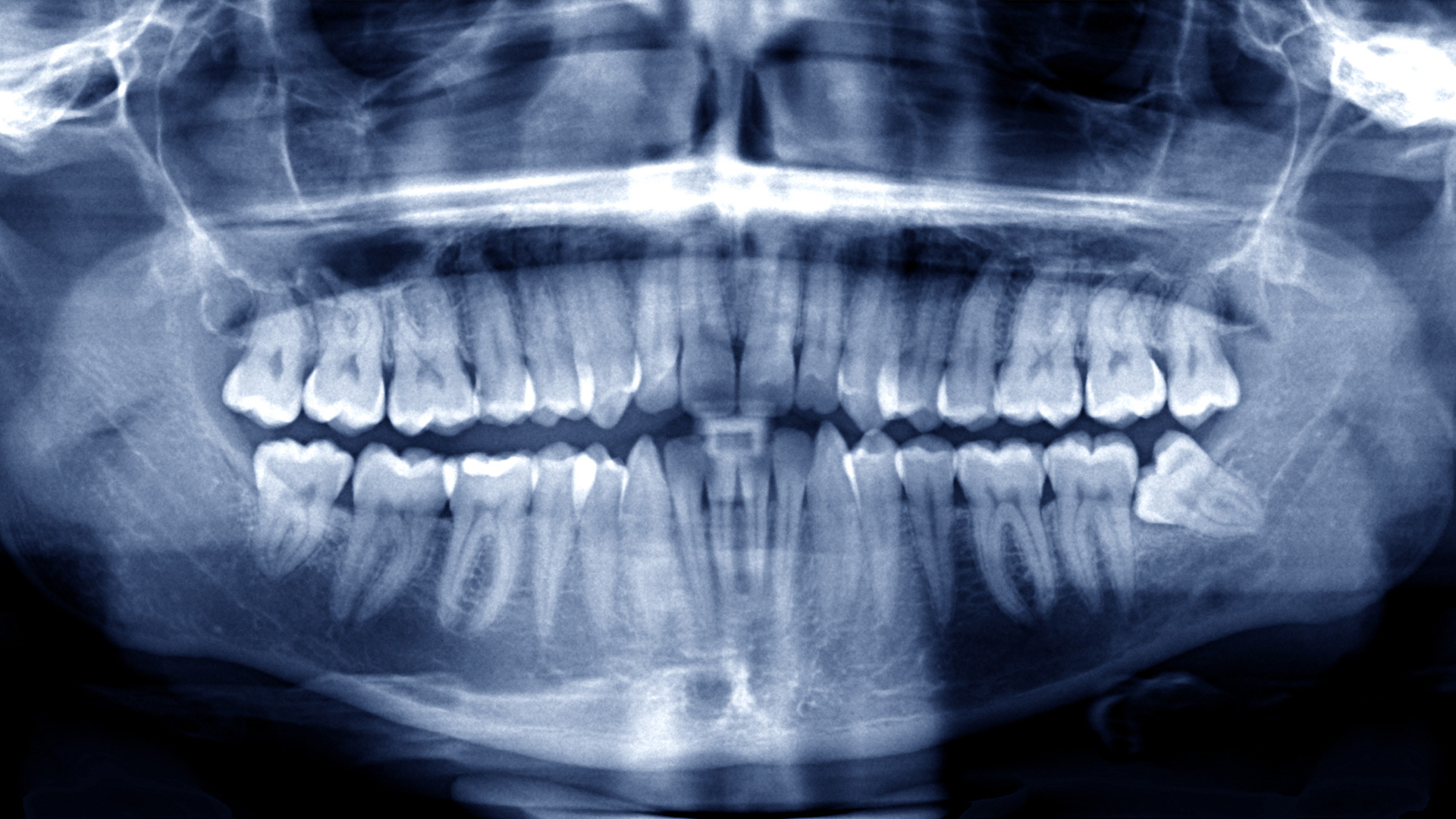
Our Philosophy on Wisdom Teeth Removal
Great improvements in dentistry now allow wisdom teeth to be a gentle, comfortable, and easy experience for the patient. Some need to be removed and some don’t, so let our experienced team of doctors help educate you on whether or not your wisdom teeth are in trouble. Every patient needs a customized evaluation of their teeth to determine if they need to be extracted, and the earlier this evaluation occurs the better. Never wait until a wisdom tooth starts to hurt! This often means that irreversible damage already exists due to infection of the adjacent bone and gum tissue.